Michael O’Dwyer
Professor of Haematology, NUI Galway and Director, Blood Cancer Network Ireland
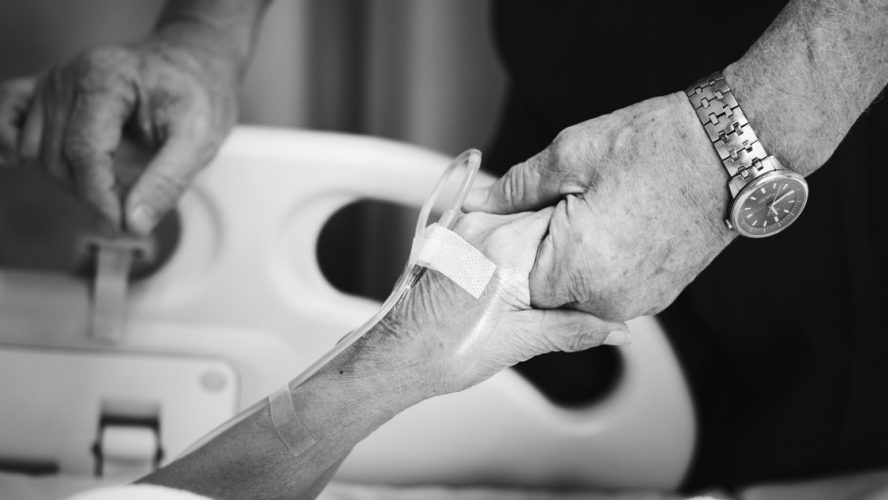
Anaemia, bone damage and kidney failure characterise Multiple Myeloma in Ireland. It is the second most common malignancy involving cells originating within the bone marrow. Irish blood disease.
Generally a disease of older patients, one third of Multiple Myeloma in Ireland are younger than 65 years of age at diagnosis. It is preceded by a pre-myeloma state in some cases. However, the role of early intervention in these cases is still unclear.
Research and development has led to a significant improvement in the survival of patients. Intensive research and successive clinical trials have led to incremental advances in survival of patients with myeloma. This is despite once having a relatively poor prognosis and limited treatment options.
25 years ago, the average life expectancy of a newly-diagnosed patient was three years
Treating Multiple Myeloma in Ireland
Traditional chemotherapy was the mainstay of treatment. While effective at controlling the disease and improving survival, chemotherapy alone rarely put patients into remission. Around this time, it was discovered that high doses of chemotherapy could induce much deeper responses. This lead to a significant minority of patients for the first time achieving remission.
Since high doses are also toxic to the normal bone marrow, this necessitated the reinfusion of the patient’s own healthy stem cells following the chemotherapy to regenerate the bone marrow. These so-called autologous stem cell transplants led to a significant improvement in the survival of patients; the first major advance in the treatment of myeloma for many years.
By the end of the 1990s, a succession of new, so-called “novel-agents” entered clinical trials for myeloma.
Drugs including proteasome inhibitors and immune modulatory drugs (IMiDs), had very different mechanisms of action to traditional chemotherapy.
The successful incorporation of these agents into treatment protocols, with and without ASCT, has been a huge success in the treatment of myeloma. Coinciding with their introduction, there has been a steady improvement in the overall survival and quality of life of patients with myeloma, including in Ireland, such that 50% of newly diagnosed patients now live five years or more.
Despite advances, there is no room for complacency
When breaking down Irish blood disease according to age, it is clear that younger patients have derived the greatest benefit.
There is abundant evidence now that those patients achieving the deepest responses – where even sub-microscopic is no longer detectable – enjoy the longest remissions and best survival. This is referred to as Minimal Residual Disease (MRD) negativity and this is now a major goal of treatment.
Standard treatment now involves transplant. Patients under the age of 65 now have a 50% chance of surviving. Studies have shown at least seven years and in excess of 10 years. This is a huge change from the 1990s.
However, Multiple myeloma in Ireland remains largely an incurable disease. In most cases, it eventually comes back and ultimately proves resistant to therapy. Early relapse and resistance is more likely for the 20-30% of patients who have certain poor risk features, typically based on genetic analysis. Even our best standard therapies are often insufficient in these patients, highlighting the need for new treatment options.
Funding is vital for (CAR)-T therapy in Ireland
Thankfully, a number of promising new drugs have either recently been approved or are being tested in clinical trials.
New strategies, which engage the immune system, appear particularly promising. Among these are monoclonal antibodies and chimeric antigen receptor (CAR)-T cell approaches. Many of these new treatments are very expensive, however, and pose a major financial burden for the health service as well as representing a barrier to patient access.
Our once excellent survival rates in Ireland were due to having the best access to myeloma drugs in Europe. However, in recent years, approvals of new myeloma drugs in Ireland has lagged behind other European countries. To avoid sliding further down the international rankings, we require a more robust, transparent approval process.
Clinical trials have a very important role to play too. They enable access to drugs that might not otherwise be available as well as huge cost savings. With limited resources, Blood Cancer Network Ireland and Cancer Trials Ireland have made a vital contribution in making exciting new therapies available to myeloma patients in Ireland.
Strategic investment, embedding clinical cancer research within our healthcare system could pay huge dividends, putting Ireland on the map internationally, but most of all benefiting patients.